Since our founding in 2011, Sendero has sought to provide value-adding services to our members and the community that are not found in traditional for-profit health plans. As this timeline illustrates, Sendero’s made valuable contributions to the communities we serve and we are proud in turn of the support we receive from our community. As we prepare for our next decade of service to Travis and surrounding county residents, we reaffirm our commitment to supporting the health of our community by providing affordable, quality healthcare coverage.
Sendero is the first area ACA Plan to waive the cost of treatment and diagnosis to all members. Outreach completed to more than 1,000 high-risk members and offered payment plans to members in financial distress from pandemic.
Distributed 12,000 COVID-19 and Flu Care Packages to members and community.
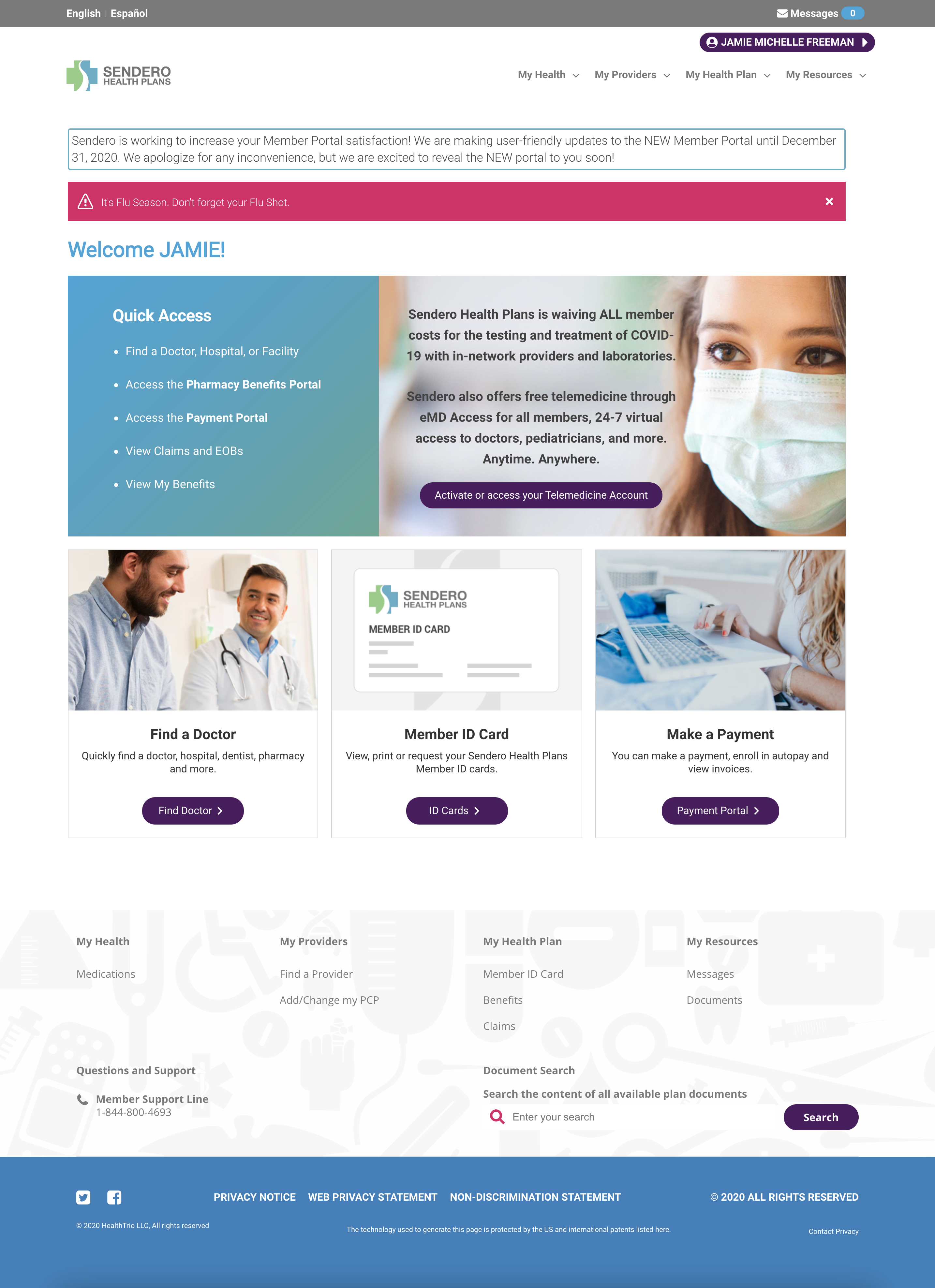
Providing Sendero members with a central hub to connect them with all the personalized tools they need in one place.

Launched program to provide "Swan Songs" by having local musicians play for hospice patents.
Sendero receives a $25,000 donation from the estate of a Sendero member to support the CHAP program and provide coverage for chronically ill patients.
Sendero is 1 of only 2 out of 17 STAR/CHIP Medicaid plans to receive A rating.

Sendero makes telemedicine through eMD Access a 100% free benefit for all members.

Began hosting Free Family Movie Nights in the community with health information and fun activities for the whole family.

Recognized as Top Workplace by the Austin American Statesman. Received recognition in 2018 and 2020 as well.

Sendero Sponsored field trips for kids from 12 area Title I schools and paid for the transportation and admission at the Aquarium, Thinkery, Austin Zoo, and the Bob Bullock Museum.

Began providing transportation assistance for pregnant mothers to birthing classes, Sendero's birthing classes, WIC appointments, and other Sendero A Tu Lado events.

Under an initiative launched by President Barack Obama, Sendero provided free disposable diapers to low-income mothers in Central Texas who participated in Sendero's A Tu Lado program. Qualifying Sendero members were had free diapers shipped directly to their homes thanks to a partnership created by the White House with Cuties diapers and Jet.com.

Sendero’s program provided maternity services and care for expecting mothers, including free pregnancy testing services, free diapers, and baby showers. Sendero’s Community Health Workers accompanied members every step of the way from pregnancy testing through delivery and beyond to ensure that pregnant women could access all appropriate services available to improve the health of both mom and baby. In addition to the free testing and practical care items, Sendero provided educational materials and a host of other services, including gift cards for Well Child checks and new member assessments and information on free meals for children at area restaurants.

Partnered with City of Austin Parks and Recreation to encourage an active lifestyle and the pursuit of athletics for kids ages 8-18 by providing them with an opportunity to visit and train with Leo Manzano, an 2012 Olympic Medalist and Austin resident.

Sendero provided sponsorship and support for the Eagle Talk Show, a television program produced by Austin ISD which provided health and wellness information for AISD parents. The show often featured Sendero and other community leaders discussing practical and meaningful ways for parents and students to thrive in their health and academic progress.

A bilingual, 36 page custom print magazine highlighting programs, partnerships, health plan coverage and individuals or community organizations that are model examples and advocates of healthy living. 100,000 copies of the magazine were distributed quarterly to selected faith-based groups, medical offices, retail stores such as HEB and CVS, and school districts within the 5-county area.

Began providing access musicians and other Central Texans in need of affordable health care with Central Health covering the premiums. In 2018, expanded the program to access millions of dollars of Affordable Care Act funds and provide health insurance to chronically ill patients. This highly successful program enables CHAP members to access greater care options, such as dialysis, that was previously unavailable. “it has been wonderful for us,” said one enrollee. “It just eases my mind knowing that there is support, especially for artists like me. Knowing my family has health insurance allows me to focus on my work. I know many other artists who feel the same way.”

Partnered with AISD on a campaign to promote College Ready and PreK enrollment throughout the district.
Sendero gains National Center for Quality Assurance (NCQA) Accreditation, meaning Sendero supports care that keeps members at optimum levels of health while controlling their costs and meeting government and purchaser requirements.


Sendero staff participated in Dell Children's 5K benefitting the Texas Center for the Prevention and Treatment of Childhood Obesity.

Sendero began covering enrollment costs for participation in one youth sports session per season for Sendero members 2 ½-18 years of age. This made free swim lessons and other sports programs available for Sendero families who might not otherwise have been able to participate.

Began offering health plans through the Affordable Care Act marketplace that has resulted in more than 100,000 central Texans insured through 2020.

When we learned of Coach Juan Lopez's soccer team made up of kids in the Montopolis neighborhood, we were inspired to step in and sponsor the program. Before Sendero sponsored the Dragons, they were playing with borrowed equipment and makeshift uniforms. We partnered with Allison Elementary School for the program and at the end of their victorious season, Sendero held an awards banquet and honored each team member with a trophy.

Began covering enrollment for participation in YMCA youth sports for members 5-14 years of age and the full cost of Boys & Girls Clubs memberships for members in Travis, Bastrop, Hays, Williamson counties.

When a historic flood-damaged homes and displaced families in the Dove Springs neighborhood on Halloween night, Sendero provided 100 care packages to the community, each package containing a grocery gift card, blankets, towels, socks and other basic items.

In an effort to reduce emergency room visits, Sendero launched a pilot program that sent licensed community health workers with the Latino Healthcare Forum to homes of Spanish-speaking parents who need help understanding what the doctor recommended.

Kicked off annual sponsorship for flu vaccine and flu season awareness event that occurs near Halloween each year, delviering nearly 2,000 free flu shots through 2020

Sendero began offering Medicaid plans to low-income Central Texans.
PO Box 759, Austin, TX 78767
© Copyright Sendero Health Plans 2024
All Rights Reserved.
Attention: This website is operated by Sendero Health Plans and is not the Health Insurance Marketplace® website at HealthCare.gov. This website does not display all Qualified Health Plans (QHPs) available through HealthCare.gov. To see all available QHP options, go to the Health Insurance Marketplace® website at HealthCare.gov. Also, you should visit the Health Insurance Marketplace® website at HealthCare.gov if you want to enroll members of your household in separate QHPs.